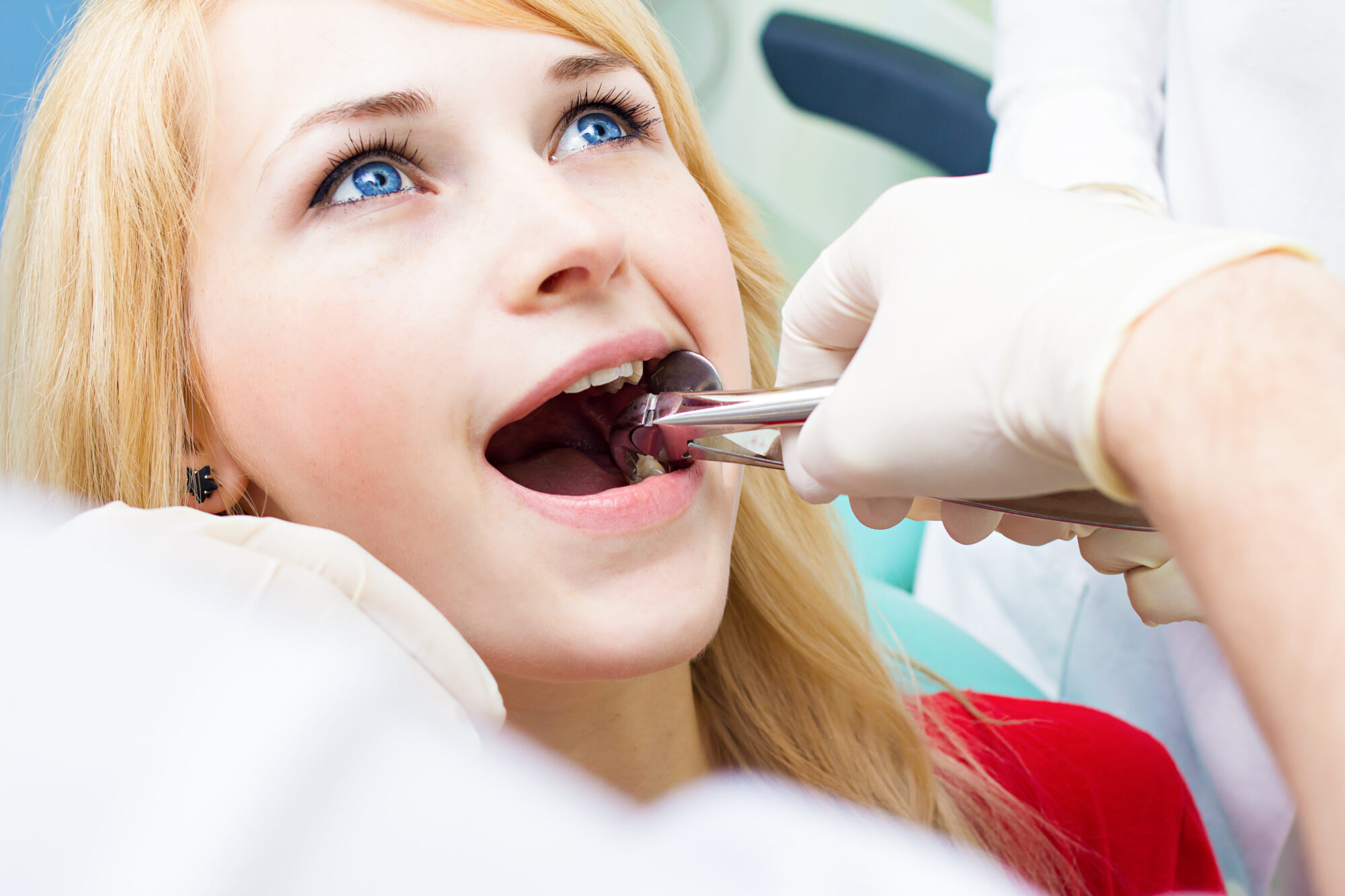
Extracting a tooth is a standard dental procedure. Most Americans will experience an extraction at least once in their life. Unfortunately, in about 5% of standard extractions and about 35% of wisdom tooth extractions, the patient also ends up suffering from a dry socket.
A dry socket occurs when the protective blood clot that forms when a tooth is removed breaks loose from the gum, leaving an open wound in the patient’s jaw. The socket can expose bone and nerve tissue, leading to excruciating pain that can radiate from the mouth into the entire upper body.
No matter who you are, but especially if you’ve suffered from a dry socket before, you may wonder how quickly after an extraction you can stop worrying about the possibility of developing a dry socket.
This month, we’ll answer that and other questions that we’re commonly asked about dry sockets so that you can face your next oral procedure with confidence.
When Can I Stop Worrying About Dry Socket?
A dry socket is only a concern for as long as it takes for your mouth to heal after an extraction. For most patients who’ve had a tooth extracted, that healing should take between seven and ten days.
Once the wound has healed, the blood clot from the extraction is no longer required to shield the underlying tissue, and the risk of a dry socket goes away completely. You can tell when your oral wound has healed when your gums are no longer swollen or tender. If you can see the affected site, you’ll be able to see that the skin of the gums has entirely closed over the top of the wound, and none of the dark blood clot is visible.
Some studies have suggested that the healing of oral wounds may take longer for some individuals. In general, men’s mouths tend to heal quicker than women’s, and healing is slower in older individuals.
Are Certain People More at Risk for Dry Sockets?
There are a number of risk factors associated with dry socket, some of which are uncontrollable, and some of which are lifestyle factors that can be addressed to reduce your risk.
Uncontrollable Risk Factors:
- History of dry socket – If you’ve experienced a dry socket before, you’re more likely to experience it after future extractions.
- Oral infection – Patients with infections in the mouth are more likely to experience a dry socket.
- Traumatic or difficult extractions – A complicated extraction that causes more than the typical damage to the jaw or gums is more susceptible to a dry socket.
- Jawbone issues – There are a number of conditions of the jaw that can put patients at a higher risk of dry socket.
Controllable Lifestyle Factors:
- Smoking – Patients who smoke are more likely to suffer from almost every possible medical problem and complication, including dry sockets. If you smoke, quit. If you don’t, don’t start!
- Contraception – Oral contraceptives can increase the risk of a dry socket.
- Other medications or supplements – Some medications and supplements can lead to slow or hampered clotting and make the risk for a dry socket much higher.
- Poor dental hygiene – Brushing and flossing daily and getting regular checkups at the dentist are the best ways to reduce your risk for dry sockets. Dry socket risk is directly related to oral health, and dental hygiene is the pathway to good oral health.
Are Certain Extractions More Likely to Cause Dry Socket?
Yes, certain types of extraction have higher dry socket risks than others:
- Extractions from the lower jaw are more likely to result in a dry socket than extractions from the upper jaw.
- Extractions in the back of the mouth tend to have higher rates of dry sockets than those in the front of the mouth.
The extraction of lower wisdom teeth is the highest-risk standard dental extraction. Research indicates that a third or more of all lower-jaw wisdom tooth extractions result in a dry socket.
Is There Anything I Can Do to Prevent a Dry Socket?
Absolutely! For details, you can look back at last month’s article, but in brief:
- Use cold packs, painkillers, or other means of controlling your pain and inflammation.
- Limit your activity and avoid high-impact activities that can jar the clot loose.
- Avoid using straws – the suction created by sipping through a straw is enough to dislodge a clot.
- Avoid crunchy or chewy foods and stick to a soft diet until your mouth has healed.
- Gently rinse your mouth with a salt solution several times a day.
Can a Dry Socket Lead to Other Complications?
It’s not typical for a dry socket to lead to additional complications – which is good because the pain and discomfort are more than enough to deal with. However, there is a slight risk that a dry socket will serve as an entry point for an infection.
Beyond that, the pain from the dry socket can lead to other indirect complications, including loss of sleep, inability to eat, and others.
If you do experience a dry socket, you should contact your dentist or oral surgeon immediately. They’ll be able to take a number of steps to reduce your pain, prevent any secondary infections, and get your mouth back on the road to healing.
Athens Oral Surgery Is Your Local Oral Surgeon With More Than a Decade of Experience.
Dr. Tomlinson and his team can perform any necessary extractions and provide you with excellent aftercare instructions to help you avoid a dry socket or comprehensive care in the event that you develop a dry socket. Schedule an appointment by calling 706-549-5033.
Related Articles:
